Access to health services in Shepparton is improving, study finds
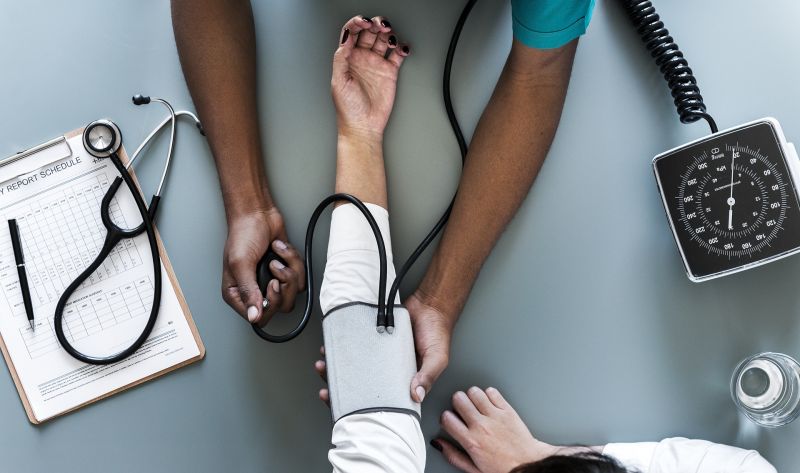
Expansion and improvement of healthcare services in Shepparton over the past 15 years has led to an increase in use, according to the latest Crossroads Research Study key findings.
Led by the University of Melbourne’s Department of Rural Health, the Crossroads project is one of most detailed health studies undertaken in rural Australia, designed to understand the prevalence of chronic health conditions in the Goulburn Valley and community needs.
Around 1800 households were randomly selected in Shepparton and Mooroopna to take part in the study. Of these, just over 900 households participated with 1344 adults completing a detailed health questionnaire.
Since the original study in Shepparton and Mooroopna was conducted in 2001-2003, the use of services has increased, with 93 per cent of participants surveyed 2016-2018 visiting a GP in the past year. Satisfaction has also increased, with 90 per cent of participants satisfied with their GP, medical specialists and hospital care.
University of Melbourne rural health expert Lisa Bourke said the ultimate aim of the project is to see health services not only improved, but better tailored to what the local community needs and wants.
“By understanding more about community needs and the barriers to care, we can help local providers identify gaps, make strategic decisions for their health services and build cases for funding,” Professor Bourke said.
The study found that in the past 15 years there has been a decrease in undiagnosed disease, demonstrating that more people are having regular health screenings such as blood pressure, skin and cancer checks. Rates of smoking have declined to 14 per cent, which is much lower than the earlier study (22 per cent) and lower than the state average
Immunisation has also increased with 94 per cent of participants saying they had been immunised for childhood diseases, an increase of 86 per cent from 2001-2003.
Although there have been positive gains since the original study, rates of chronic and long-term conditions have increased.
68 per cent of people surveyed indicated they were overweight, an increase since 2001-2003 and above state average. Social isolation and loneliness were also identified as key issues, particularly among the elderly.
“Consistent with studies in other regions, these concerns remain an area of focus,” Professor Bourke said. “We are working with local health services to develop models that work with the population and promote a whole-of-community approach to health living that expands current strategies.”
Goulburn Valley Primary Care Partnership executive officer Craig Chadwick said these studies are vital in rural environments to ensure service planning is based on robust data.
“We need localised, real time data that reflects the health status, emerging needs and services gaps in our communities,” Mr Chadwick said.
The Crossroads project is delivered in partnership with local health services, hospitals and governments.
The research team extend their sincere thanks to all of the participants who made this study possible – giving up their time and sharing vital information to improve local health services and drive evidence-based decision making.
People are invited to attend a community feedback session about the key findings on Tuesday, 4 June at 12pm held at the University of Melbourne Department of Rural Health, 49 Graham Street Shepparton VIC 3630.